The “Baby Blues” is a ubiquitous term for the self-limited, dreary, teary days that up to 80% of mothers experience in the first week postpartum (Williams, 2014). It is also well-known, and recognized, that Postpartum Depression (PPD) is a clinical condition requiring recognition, treatment, and ongoing support. Thankfully, there are many resources, networks, and tools available to guide women through a dark postpartum chapter. However, lesser supported, I argue, is Major Depressive Disorder in pregnancy (MDD). Perinatal Services of BC estimates that up to 1 in 5 women will experience an episode of depression in their pregnancy (Williams, 2014). While this rate is similar to the non-pregnant population, the clinical significance of depression during pregnancy is heightened, with implications for both mother and baby.
I feel MDD in pregnancy can be best illustrated through a socioeconomic model of health. The socioeconomic model is a multilevel model, or approach, to understanding health. It goes beyond the individual to explore what organizational, and social structures impact a given health issue. As Galea describes, it asks about the relationship between lifting a law that requires motorcyclists to wear a helmet and head injuries (2015). This is in contrast to the impact on the relationship between an individual rider not wearing their helmet, and head injuries – a single level approach (Galea, 2015). What I appreciate about the multilevel model, is that it identifies associations that are difficult to gather, or provides insights into the nuances of health issues not obtained through a single level analysis. I feel this is important, because it provides a framework for which we can explore health issues, but also create programs, policies, and objectives that have long reaching effects. Let’s dive in to looking at depression in pregnancy from each level.
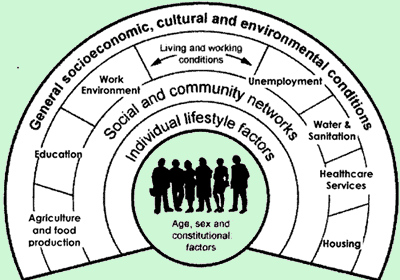
Individual Lifestyle Factors
Many approaches to treating and preventing MDD include “self-care” strategies. Behaviours such as exercise, sleep, and nutrition are usual suspects. We can lump these under Cognitive Behavioural Therapy, or CBT. While pre-pregnant/postpartum women may succeed in these strategies, pregnancy challenges a woman’s ability to exercise, sleep, and eat as she usually would. This can be due to nausea, insomnia, and discomforts associated with increasing gestation. Furthermore, women who have pre-pregnancy lifestyles that include behaviours such as smoking, drinking alcohol, or using other substances, may dramatically change their lifestyle, removing addictive substances that were previously used for coping. All of these lifestyle changes could theoretically place women at higher risk of experiencing MDD. Moreover, women may us alcohol, cigarettes, or other substances to cope with their symptoms (Williams, 2014). For women who are depressed, this would further provide challenges to participating in CBT activities, and reduce the effectiveness of some medications (Haring, 2011).
Social and Community Networks
Pregnancy represents one of the largest transitions in a woman’s lifetime. Having a baby will strengthen some relationships, and challenge others. Friendships may be strengthened through reliance on friends with children for support and guidance, where other friendships may fizzle as interests begin to diverge. For couples expecting a baby, discrepancies over finances, or parenting styles can cause conflict. In fact, over 25 studies show that marriage quality drops in the transition to parenting, often precipitously (Medina 2014, Belsky,1990). Undoubtedly, relationship or family conflict is a risk factor for MDD (Williams, 2014).
For some women, pregnancy is unintended. An unintended pregnancy will also create changes in the relationships with those closest to her. If the father of the baby is not involved, she faces a soon-to-be reality of functioning in the world as a single mother. While there are women who intentionally, and with empowerment, embark on single parenting through reproductive technologies, for many single mothers, this change in their social networks may increase their risk of depression (Williams, 2014).
Living and Working Conditions
Work environment, housing, and access to healthcare services may impact a woman’s risk of MDD in pregnancy (Williams, 2014, Lovisi, 2005). In caring for low-income women, I have seen that maintaining employment, housing, and attending prenatal appointments can be met with obstacles. Towards the end of their pregnancy, some struggle to meet the physical demands of their jobs, while trying to meet requirements for maternity leave. Housing can be overcrowded, or substandard, with concerns for the new baby’s wellbeing at the forefront of the mother’s mind. This includes the fear of involvement from the Ministry of Children and Family Development. Lastly, attending prenatal visits can be a hidden cost for pregnant moms. Reliance on public transit, or finding rides can require cash, time, childcare, and reduced work hours.
General Socioeconomic, Cultural, and Environmental Factors
At this level, there is a need for further research. A systematic review from Scotland concluded that the evidence doesn’t support specific interventions for the prevention of MDD during pregnancy, unless identified risk factors are present (SIGN, 2012). I argue that this is short sighted. While it factors in a woman’s personal and family medical history, and contributing risk factors from individual, social, living conditions factors, it fails to consider general socioeconomic, cultural, and environmental factors as risk factors for, or associations with, depression in pregnancy. For example, it does not include exploration of concepts such as how colonialism may impact pregnancy MDD rates among Aboriginal women, or how cultural norms around “motherhood” and the identity of “mother” may contribute to MDD. Using a socioeconomic model to further explore depression in pregnancy, may allow us to discover evidence that does support specific interventions for prevention for specific populations. Ultimately, our guidelines are only as good as the literature used to create them.
References
Alio, A., Richman, A., Clayton, H., Jeffers, D., Wathington, D., & Salihu, H. (2010). An ecological approach to understanding black-white disparities in perinatal mortality. Maternal & Child Health Journal, 14(4), 557-566. doi:10.1007/s10995-009-0495-9.
Belsky, J., and M. Rovine. (1990) Patterns of Marital Change across the Transition to Parenthood: Pregnancy to Three Years Postpartum. J of Marr & Family 52: 5-19.
Fisher, M. (n.d.). Health and socio-economic equalities. Retrieved from http://www.self-willed-land.org.uk/permaculture/health_ineqs.htm
Galea, S. (2015, March) The Determination of Health Across the Life Course and Across Levels of Influence. Boston University School of Public Health. Retrieved from https://www.bu.edu/sph/2015/05/31/the-determination-of-health-across-the-life-course-and-across-levels-of-influence-2
Haring, M. (2011, February). Coping with depression during pregnancy and following the birth: A Cognitive-Behaviour Therapy-based self-management guide for women. Retrieved https://reproductivementalhealth.ca/sites/default/files/uploads/resources/files/coping_with_depression.pdf
Lovisi, G., Lopez, J., Coutinho, E., & Patel, V. (2005). Poverty, violence and depression during pregnancy: A survey of mothers attending a public hospital in Brazil. Psychological Medicine, 35(10), 1485-1492. doi:10.1017/S0033291705005362
Medina, J. (2014). Brain rules for baby: How to raise a smart and happy child from zero to five. Brunswick, Melbourne, Vic.: Scribe Publications.
Scottish Intercollegiate Guidelines Network (SIGN). (2012, March). Management of perinatal mood disorders. Edinburgh: SIGN; 2012. (SIGN publication no. 127). Retrieved from http://www.sign.ac.uk
Williams, J. (2014, March). Best Practice Guidelines for Mental Health Disorders in the Perinatal Period (Canada, Perinatal Services of British Columbia). Retrieved from http://www.perinatalservicesbc.ca/Documents/Guidelines-Standards/Maternal/MentalHealthDisordersGuideline.pdf
